2026 Top Trends in Orthopedic Surgical Outcomes You Need to Know?
As we approach 2026, the landscape of orthopedic surgical outcomes is evolving rapidly. Innovations in technology and surgical techniques are reshaping how surgeries are performed. Surgeons are leveraging data analytics to enhance decision-making and improve patient outcomes. However, these advancements also raise questions about consistency and applicability across different demographics.
In the realm of orthopedic surgeries, patient safety remains a top priority. Despite the advancements, complications can arise, leading to varying outcomes. Understanding these potential pitfalls is essential for both practitioners and patients. Personalized treatment plans are becoming vital, as what works for one patient may not work for another. An individualized approach aims to address these concerns and improve overall effectiveness.
Engaging in transparent discussions about orthopedic surgical outcomes is crucial. Patients should be educated about potential risks and benefits. Reflecting on past outcomes can guide future practices. A comprehensive understanding of these trends will empower patients and healthcare providers alike, ensuring a more informed decision-making process in the surgical journey.

Emerging Technologies Enhancing Orthopedic Surgical Precision in 2026
Emerging technologies are revolutionizing orthopedic surgery in 2026. Innovations like robotic-assisted systems improve precision. These systems allow surgeons to navigate complex procedures with enhanced accuracy. The integration of artificial intelligence aids in pre-operative planning. AI can analyze patient data for optimal surgical strategies.
Robotic platforms are transforming traditional methods. These machines can execute tasks with minimal invasiveness. Surgeons report reduced recovery times for patients who undergo robotic procedures. Virtual reality is being used for training young surgeons. It simulates real-life scenarios, improving skills before they enter the operating room.
Tips: Stay informed about the latest technologies. Attend workshops and seminars on surgical advancements. Engage with healthcare professionals to discuss experiences with new tools. Consider how these innovations might enhance your practice and patient outcomes. Always reflect on your methods and remain open to change. Embrace the future of orthopedic surgery with a critical eye.
Data-Driven Insights: The Role of AI in Predicting Surgical Outcomes
In 2026, artificial intelligence (AI) is set to transform orthopedic surgical outcomes. Predicting results has traditionally been a complex task. However, recent advancements in AI offer more precise predictions. By analyzing vast datasets, AI can identify patterns in patient outcomes. This data-driven approach enhances decision-making in surgical planning.
The integration of AI in orthopedic surgery raises important questions. How accurate are these predictions? Can they account for individual patient factors? While AI shows promise, it is not infallible. Challenges remain in ensuring consistently reliable data. Moreover, reliance on AI could lead to overlooking valuable clinical insights from experienced surgeons. Balancing technology with human expertise is crucial for improving patient care.
As AI continues to evolve, its role will likely grow. For orthopedic surgeons, staying informed about AI advancements is essential. Engaging in discussions about its ethical implications is equally important. Understanding AI's limitations will lead to better surgical practices. This evolving landscape will shape the future of orthopedic surgery significantly.
Patient-Centered Approaches: Customization in Orthopedic Procedures
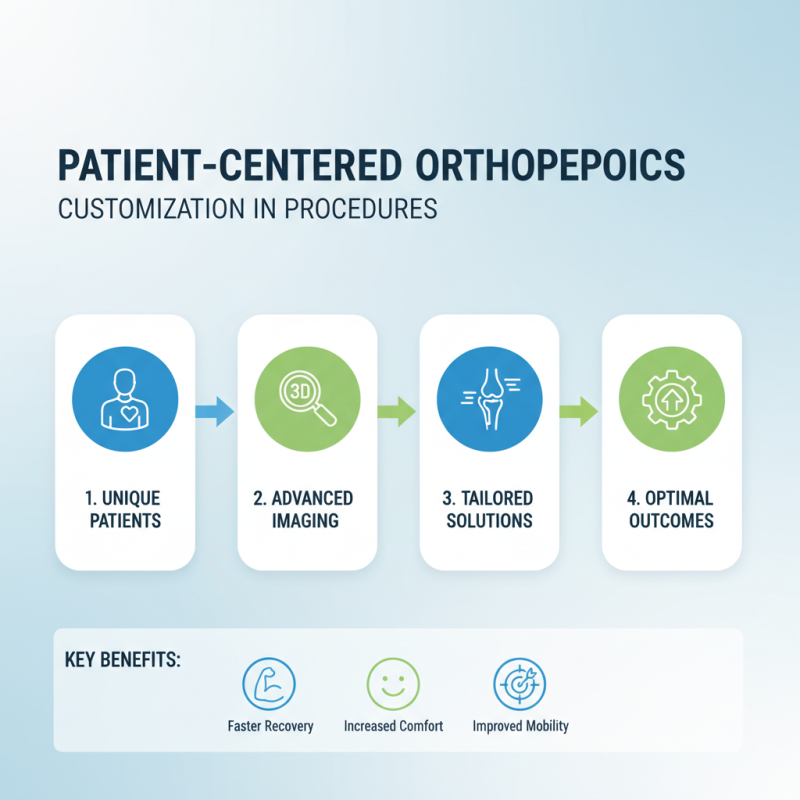
In recent years, the focus on patient-centered approaches in orthopedic surgery has gained significant traction. Customization is becoming a key aspect of orthopedic procedures. This shift recognizes that each patient is unique, requiring tailored solutions to achieve optimal outcomes. Surgeons are increasingly using advanced imaging technology to better understand individual anatomies. By doing so, they can create personalized plans that align with the specific needs and goals of each patient.
However, this approach is not without challenges. There are ongoing debates about the efficacy of highly individualized procedures. While many patients report better satisfaction, some studies suggest variability in surgical outcomes. The balance between standardization and personalization remains a topic of reflection within the field. Surgeons must weigh the benefits of customization against the risks involved, including longer surgery times or increased costs. As the orthopedic landscape evolves, embracing the patient’s voice in the treatment process is essential, but ongoing evaluation of these methods is critical.
Ultimately, the success of customized orthopedic surgery hinges on collaboration between patients and healthcare providers. Open dialogue can help identify realistic goals and expectations. This partnership fosters trust and can enhance recovery experiences. As we move toward 2026, the focus on tailored orthopedic solutions will redefine patient satisfaction and surgical outcomes.
Postoperative Recovery Trends: Optimizing Rehabilitation Success Rates
Postoperative recovery is crucial for orthopedic surgical success. A focus on rehabilitation trends can significantly improve patient outcomes. Innovations in physical therapy techniques are emerging. These methods emphasize personalized care, addressing individual needs and recovery goals.
Tips: Incorporate mobility exercises early. Begin gentle stretches to maintain joint flexibility. This can reduce stiffness and promote healing in the early stages.
Nutritional support also plays a vital role. A well-balanced diet speeds up recovery. Essential nutrients like protein and vitamins aid in tissue repair. Patients should consult with nutritionists for tailored meal plans.
Tips: Stay hydrated throughout recovery. Water supports metabolic processes and overall health. It aids in managing pain and inflammation, providing patients with a better recovery experience. It's not just about exercising; lifestyle choices matter deeply.
2026 Top Trends in Orthopedic Surgical Outcomes: Postoperative Recovery Trends
Minimally Invasive Techniques: Reducing Complications and Enhancing Outcomes
Minimally invasive techniques have transformed orthopedic surgery. These methods significantly reduce patient recovery time and lower complication rates. According to a recent industry report, minimally invasive surgeries can decrease hospital stays by 30% and complications by up to 50%. This is crucial for improving surgical outcomes and patient satisfaction.
Surgeons employing these techniques often utilize advanced imaging and robotic assistance. These tools enhance precision and reduce soft tissue trauma. However, some surgeons may hesitate to adopt these methods. They worry about the steep learning curve and initial setup costs. It is essential, though, to weigh these concerns against the long-term benefits provided to patients.
Tip: Stay updated with the latest training programs. Continuous education is vital for mastering minimally invasive techniques.
Another aspect to consider is patient selection. Not all patients qualify for these procedures. Careful screening is necessary to ensure the best outcomes. Complications, while reduced, still occur. Thus, it is important to establish realistic expectations for patients.
Tip: Communicate openly about potential risks and benefits before surgery. This fosters trust and enables informed decision-making.
Related Posts
-
China Top Knee Implant Technology Advancements and Innovations?
-
2026 How to Effectively Manage Post Surgery Rehabilitation Process?
-

Top Strategies for Orthopedic Mobility Restoration Techniques?
-
Top 10 Advanced Joint Implants Transforming Orthopedic Surgery?
-
How to Choose the Right Orthopedic Implant Fixation Method?
Copyright © 2021 United Orthopedic Corporation All Rights Reserved.