How to Choose the Right Orthopedic Implant Fixation Method?
Choosing the right orthopedic implant fixation method is crucial in ensuring successful surgical outcomes. According to a recent report by the Orthopedic Research Society, the global orthopedic implant market is projected to reach $45 billion by 2025. This growth highlights the significance of advanced fixation techniques. Dr. Emily Johnson, a leading expert in orthopedic surgery, emphasizes, “The choice of fixation method can drastically impact recovery time and overall patient satisfaction."
Orthopedic implant fixation encompasses various techniques that stabilize fractures and support healing. Each method has specific indications and contraindications, making selection complex. The challenge lies in evaluating factors such as bone quality and fracture type. A recent study indicated that improper fixation choices can lead to a 30% increase in complications. Stakeholders must understand both the advantages and limitations of each fixation method.
The field requires continuous improvement. Surgeons must remain updated with evolving technologies and techniques. Reflection on past cases often reveals opportunities for better outcomes. Engaging in professional development can improve decision-making. Selecting an orthopedic implant fixation method is not merely a technical task; it requires a comprehensive understanding of patient needs and clinical contexts.
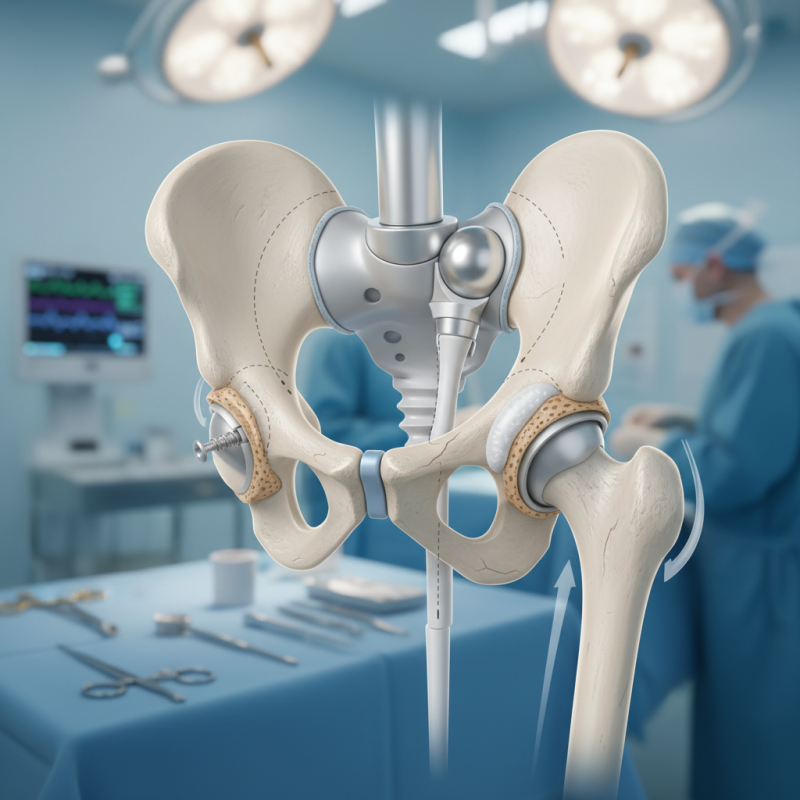
Overview of Orthopedic Implant Fixation Methods
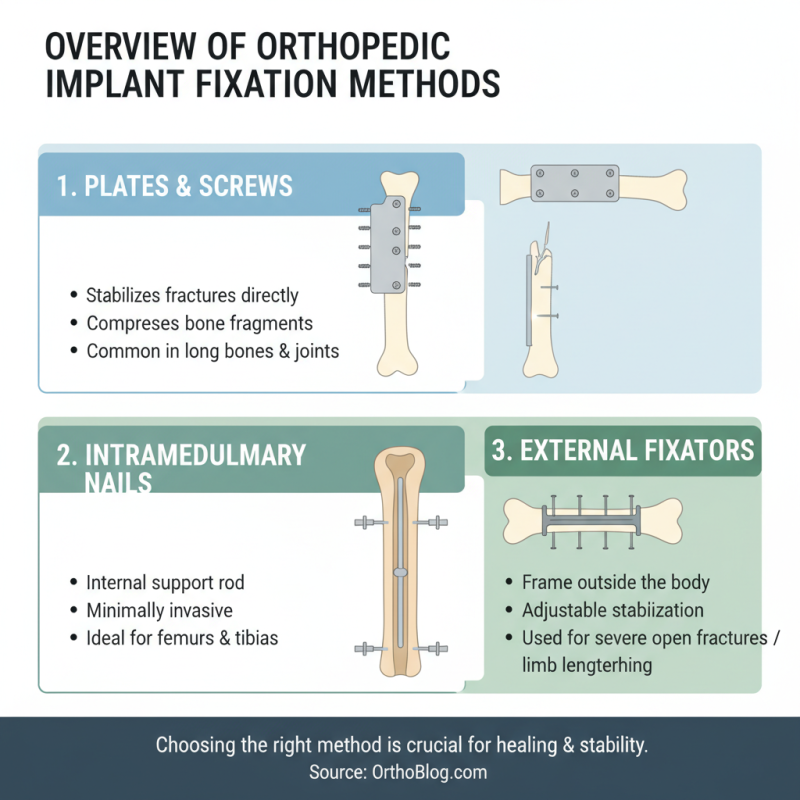
Choosing the right fixation method for orthopedic implants is crucial for successful outcomes. Several techniques are available, each with specific advantages. These methods include plates and screws, intramedullary nails, and external fixators. Each option has unique implications for healing and stability.
Plates and screws offer rigid fixation, which is beneficial for fractures that need precise alignment. However, this method may require extensive soft tissue dissection. Intramedullary nails provide internal support and are less invasive. They work well for long bone fractures but may not be suitable for all cases. External fixators are useful for complex fractures or infections. They allow for easy adjustment and removal, but may lead to complications like pin site infections.
Surgeons must weigh these options carefully. The patient's specific condition plays a vital role in selection. Understanding the advantages and drawbacks of each method can be challenging. Communication between the surgeon and patient is essential for informed decisions. An awareness of the potential complications is necessary for effective treatment planning.
Factors to Consider When Selecting Fixation Techniques
Choosing the right fixation method for orthopedic implants is critical. Surgical outcomes depend heavily on various factors. Surgeons must evaluate the patient's age, activity level, and bone quality. For instance, a study published in the Journal of Orthopedic Surgery revealed that younger patients with high activity levels often benefit from more rigid fixation methods.
The type of bone fracture also plays a major role. Complex fractures might require hybrid techniques to enhance stability. According to the American Academy of Orthopaedic Surgeons, approximately 76% of surgeons reported selecting fixation techniques based on fracture type and associated risks. Additionally, implant material quality is crucial. Biocompatibility affects healing times and reduces the risk of infection.
Surgeons frequently face challenges in selecting the ideal approach. Personal experience and preferences can cloud judgment. Constantly evolving techniques complicate decision-making. Ensuring the selected fixation provides optimal stability can allow for better patient outcomes. Engaging in multidisciplinary discussions can lead to more informed choices. Clinical guidelines should be consulted, but flexibility in approach is essential.
How to Choose the Right Orthopedic Implant Fixation Method?
| Factor | Considerations | Examples of Techniques |
|---|---|---|
| Patient Age | Younger patients may heal faster; older patients may have comorbidities influencing fixation choice. | Cemented vs Cementless implants |
| Bone Quality | Assess if the bone is dense or osteoporotic, which affects stability. | Screws, plates, or intramedullary nails |
| Type of Fracture | Intraarticular vs extraarticular fractures require different management approaches. | External fixation, internal fixation |
| Location of Injury | Certain body areas have unique anatomical and functional considerations. | Ankle plates, knee arthroplasty |
| Surgical Technique | Open reduction vs closed reduction may determine fixation method. | Endoscopic fixation, traditional fixation |
| Recovery Time | Consider how quickly the patient needs to return to normal activities. | Rapid recovery protocols with minimally invasive techniques |
| Cost and Availability | Budget constraints may limit options; availability of certain implants could vary. | Standard vs advanced biomaterials |
Comparison of Internal vs. External Fixation Methods
When considering fixation methods for orthopedic implants, it's crucial to understand the differences between internal and external fixation. Internal fixation relies on devices such as plates and screws to stabilize fractures within the body. This method often leads to quicker healing and less visible scarring. Surgeons typically prefer internal methods for stable fractures, where accurate alignment is critical.
On the other hand, external fixation involves placing a stabilizing frame outside the body. This method is beneficial for open fractures or when surgery poses higher risks. External fixators can also be adjusted post-surgery. However, they can lead to issues such as pin-site infections and inflammation. The choice between these methods often hinges on specific patient circumstances and fracture characteristics.
Ultimately, each fixation method has advantages and drawbacks. A careful evaluation is essential. Patients should engage in discussions with healthcare providers about the best choice for their unique situations. As techniques and technologies evolve, ongoing research and clinical experience will continue to shape these practices.
Comparison of Internal vs. External Fixation Methods
Assessment of Patient-Dependent Factors in Implant Choice
Choosing the right orthopedic implant fixation method requires careful consideration of patient-dependent factors. Factors such as age, weight, and activity level play a significant role in determining the most appropriate implant. A study by the American Academy of Orthopaedic Surgeons found that patient characteristics account for about 75% of implant selection effectiveness.
Younger, active patients may benefit from stronger, more flexible implants. Conversely, older patients or those with comorbidities may require implants with different mechanical properties. This disparity raises questions about optimal choices. Additionally, proper weight management is essential. Evidence suggests that higher body mass index (BMI) can impact the longevity of implants.
Surgeons often rely on their expertise and clinical guidelines to make these decisions. However, individual patient profiles must still guide the process. Not all situations can fit neatly into established categories. Constant reflection on evolving practices is critical. The dialogue between surgeon and patient should focus on realistic expectations and potential risks involved with varying fixation methods. Data highlighting the importance of patient engagement is growing, suggesting that informed consent leads to better surgical outcomes.
Guidelines for Postoperative Care and Monitoring
Postoperative care is crucial after orthopedic implant surgery. Following the procedure, patients often face challenges in mobility, pain management, and understanding their recovery journey. Clear communication with healthcare teams is essential. They can help patients identify signs of infection or other complications early on. Timely intervention can make a significant difference in overall recovery.
Monitoring becomes vital as healing progresses. Patients should keep a close watch on surgical sites for unusual redness or swelling. Pain should be regularly assessed and reported, especially if it increases. Engaging in prescribed physical therapy can enhance recovery but may initially feel uncomfortable. It’s normal to reflect on these discomforts and seek reassurance from medical professionals.
Education about care practices is crucial. Patients should understand how to change dressings and recognize warning signs. Regular follow-up visits allow for professional evaluations. This proactive approach fosters a sense of involvement in one's recovery. It may be easy to overlook self-care, but dedicating time to healing is important. Mistakes can happen, and reflecting on these moments can lead to better outcomes.
Copyright © 2021 United Orthopedic Corporation All Rights Reserved.