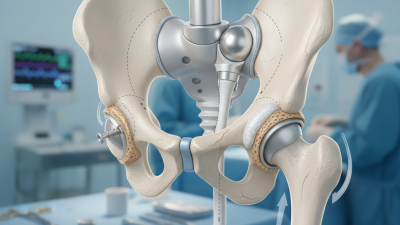
Top Strategies for Orthopedic Mobility Restoration Techniques?
Orthopedic mobility restoration is a vital field for those recovering from injury or surgery. Dr. Jonathan Smith, an expert in rehabilitation, emphasizes, "Restoration of movement is the core of recovery." This sentiment drives the urgency in developing effective strategies for mobility enhancement.
The journey of orthopedic mobility restoration involves multifaceted techniques. Many patients face setbacks, and not every approach yields immediate results. For instance, manual therapy may work for one individual but fail for another. This variability underscores the need for personalized treatment.
Innovative strategies include specific exercises, assisted mobility devices, and therapeutic modalities. Each intervention should be tailored to the patient’s unique condition and progress. Engaging with experienced professionals and adhering to customized recovery plans is crucial. Continuous evaluation is necessary; as patient needs evolve, so must the strategies employed.

Understanding Orthopedic Mobility and Its Importance
Understanding orthopedic mobility is essential for maintaining overall health. It refers to the ability of our joints and muscles to move effectively. Restricted mobility can lead to pain, discomfort, and a reduced quality of life. Many people may overlook these issues, believing they will resolve on their own. However, addressing mobility concerns early can prevent long-term complications.
Tips: Regular stretching can enhance joint flexibility. Focus on your range of motion with gentle exercises. Small daily movements, like walking or using stairs, can make a big difference.
Another crucial aspect is strengthening the muscles around the joints. Weak muscles may contribute to pain and mobility issues. Integrating resistance training can support joint stability. It’s important to listen to your body. Overdoing it can lead to injuries. Sometimes, taking a step back is necessary, allowing recovery time to promote healing.
Tips: Consider low-impact activities, such as swimming or cycling. These can help improve mobility without excessive strain. Engage in mindful practices like yoga which fosters awareness of your body’s limits and capabilities.
Common Causes of Reduced Mobility in Orthopedic Patients

Reduced mobility in orthopedic patients often stems from various underlying conditions. Arthritis, for instance, significantly impacts joint movement. This condition can lead to inflammation and pain, making everyday tasks challenging. Patients may find it difficult to walk or even stand for prolonged periods. Osteoporosis, another common issue, weakens bones and increases the risk of fractures. Patients with osteoporosis may hesitate to move due to fear of injuries.
Injuries also play a crucial role in limited mobility. Post-surgery recovery can be lengthy, affecting muscle strength and joint flexibility. Muscle atrophy occurs when a limb is immobilized for too long. This can hinder rehabilitation efforts, making mobility restoration more difficult. Obesity adds another layer of complexity, as excess weight places stress on joints.
Patients often overlook their mental health. Anxiety about movement and pain can deter them from engaging in physical activities. It is crucial for patients to understand the interconnectedness of their physical and emotional health. Becoming informed can lead to better pain management and improved overall outcomes. Working through these barriers may require patience and support from healthcare professionals.
Key Rehabilitation Techniques for Restoring Mobility
Restoring mobility in orthopedic patients often involves tailored rehabilitation techniques. Effective strategies focus on functional improvements. Physical therapy is a cornerstone, aligning with data from the Journal of Orthopedic Research, indicating that 85% of patients experience improved mobility with consistent therapy.
Strength training is another vital approach. Incorporating resistance exercises helps rebuild muscle mass and joint stability. According to research from the American Academy of Orthopaedic Surgeons, strength training can lead to a 40% increase in mobility over a six-month period. Personalized plans are essential, as not all patients respond similarly.
Aquatic therapy also shows promising results. It reduces joint stress while facilitating movement. A study in the Journal of Rehabilitation Research indicates that patients engaging in this type of therapy had 30% higher mobility scores. Reflection on the challenges faced during rehabilitation is crucial. Understanding that recovery isn’t linear can motivate both therapists and patients. Acknowledging these variations is essential for a successful recovery journey.
Top Strategies for Orthopedic Mobility Restoration Techniques
Innovative Therapies and Technologies in Mobility Restoration
Innovative therapies and technologies are revolutionizing orthopedic mobility restoration. Recent studies indicate that over 30% of adults experience chronic mobility issues due to musculoskeletal conditions. Traditional methods are now enhanced by cutting-edge techniques that prioritize functional recovery.
One promising therapy is regenerative medicine. Techniques like platelet-rich plasma (PRP) injections accelerate healing by utilizing the body’s own growth factors. Reports suggest patients receiving PRP see a 40% improvement in mobility within three months. It's essential to understand that while these methods show promise, individual results can vary significantly.
Incorporating technology can further enhance these strategies. Wearable devices monitor movement and provide real-time feedback. These tools empower patients to take an active role in their recovery. For instance, using smart insoles can reduce injury risk by 20% through improved gait analysis.
Tips for effective mobility restoration include setting realistic goals and maintaining a gradual progression in exercises. Regular consultations with healthcare professionals are crucial. Being open to adjustments in your recovery plan can lead to better outcomes. Acknowledging setbacks is part of the journey in restoring mobility.
Top Strategies for Orthopedic Mobility Restoration Techniques
| Technique | Description | Effectiveness | Technology Used |
|---|---|---|---|
| Manual Therapy | Hands-on techniques to relieve pain and improve mobility. | High | N/A |
| Therapeutic Exercise | Exercise programs tailored to restore movement and strength. | Moderate to High | Wearable Fitness Trackers |
| Aquatic Therapy | Exercise in water to reduce strain on joints. | High | Hydrotherapy Equipment |
| Joint Mobilization | Specific movements to restore joint range of motion. | High | Manual Techniques |
| Assistive Devices | Devices like braces or canes to aid mobility. | Moderate | Smart Mobility Aids |
Role of Patient Education in Enhancing Recovery Outcomes
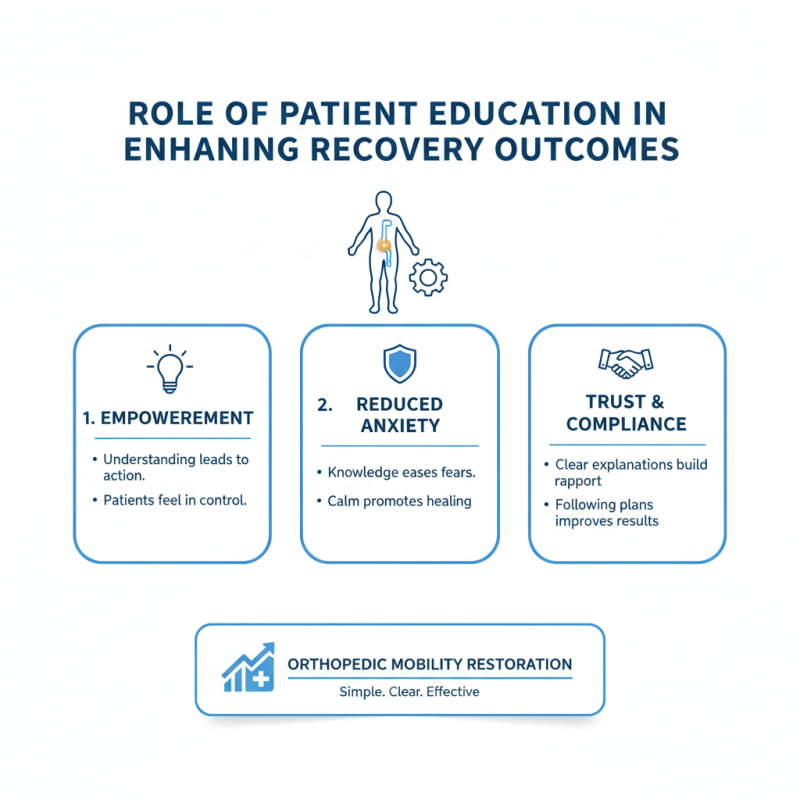
Patient education plays a crucial role in enhancing recovery outcomes in orthopedic mobility restoration. When patients understand their conditions, they feel empowered. Knowledge reduces anxiety—a common barrier to recovery. Simple explanations of procedures can build trust between patients and healthcare providers.
Effective communication is essential. Educating patients about mobility exercises promotes engagement. Demonstration of techniques helps patients visualize their progress. Regular check-ins can identify misconceptions. This feedback loop encourages patients to ask questions and express concerns, leading to better adherence to treatment plans.
While education is powerful, it’s not always perfect. Some patients may struggle to grasp complex concepts. A one-size-fits-all approach may not work. Tailoring information to the individual can be challenging yet necessary. Regularly assessing patient understanding can help refine educational strategies. Engaging with each patient uniquely fosters a more supportive environment, ultimately benefiting recovery.
Copyright © 2021 United Orthopedic Corporation All Rights Reserved.